Comprehensive Strategies to Contain Sickle Cell Disease
A COMPREHENSIVE EFFORT TO CONTAIN SICKLE CELL DISEASE
Syllabus:
GS-3: ● Science and technology in everyday life
GS-2: ● Issues related to development of social sectors like Health
Why in the News?
The National Sickle Cell Anaemia Elimination Mission (NSCAEM), launched in July 2023, aims to eliminate genetic transmission of sickle cell disease by 2047. It focuses on screening, treatment, genetic counseling, and public awareness, particularly targeting India’s scheduled tribes and other indigenous populations disproportionately affected by this debilitating hereditary blood disorder, improving healthcare access and socio-economic well-being.
UNDERSTANDING SICKLE CELL DISEASE
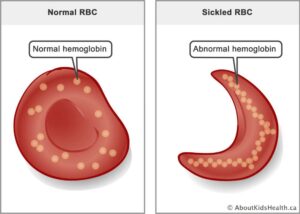
- Genetic basis – Sickle cell disease (SCD) is an autosomal recessive disorder causing red blood cells to take a crescent shape or a sickle shape, leading to reduced oxygen-carrying capacity and chronic health issues. It belongs to a group of conditions known as hemoglobin disorders, which include other conditions like hemoglobin C disease and beta thalassemia. SCD is characterized by a genetic polymorphism affecting cell hemoglobin structure.
- Disproportionate impact – Tribal communities face higher genetic prevalence of sickle cell disease combined with poor healthcare access, worsening socio-economic disadvantages. This disparity highlights the need for targeted interventions in tribal health and expanded genetic services.
- High incidence – As per the Global Burden of Disease 2021, India witnesses around 82,500 births annually with sickle cell disease, a significant share of the global sickle cell burden. This high disease burden necessitates comprehensive population screening and early diagnosis efforts through genetic screening programs.
- Chronic health toll – Patients with sickle cell anemia often endure anemia, recurrent vaso-occlusive crises, organ damage, and reduced life expectancy without timely medical care. These chronic illness manifestations can lead to acute chest syndrome, pain crises, and other severe complications. Chronic pain episodes are a hallmark of this hereditary blood disorder.
- Economic burden – Sickle cell disease leads to school dropouts, job loss, and sustained poverty cycles in already marginalized ethnic groups, particularly affecting tribal communities.
NATIONAL SICKLE CELL ANAEMIA ELIMINATION MISSION
- Mission genesis – Conceived in the Union Budget 2023 and implemented by the Ministry of Health and Family Welfare (MoHFW), with a screening target of 70 million people under 40 years by FY26.
- Ambitious goal – Elimination of genetic transmission of sickle cell disease by 2047, along with improved healthcare services for those already affected.
- Scale of operations – Considered among the largest population-based genetic testing drives globally, spanning 17 high-prevalence states.
- Comprehensive scope – Includes diagnosis, treatment, premarital counseling, awareness campaigns, and policy interventions for long-term control of sickle cell disease and related hemoglobin disorders.
- Policy continuity – Builds on the National Health Policy 2017, which identified sickle cell disease as a national public health priority.
ACHIEVEMENTS SO FAR
- Massive coverage – By July 2024, 60.7 million individuals screened, detecting 216,000 sickle cell disease patients and 1.69 million sickle cell carriers through extensive carrier screening programs.
- Concentrated cases – Nearly 95% of sickle cell disease cases located in Odisha, Madhya Pradesh, Gujarat, Chhattisgarh, and Maharashtra, predominantly affecting tribal communities.
- Medicine accessibility – Hydroxyurea included in the National Essential Drug List to ensure free and consistent supply to sickle cell disease patients, improving treatment options and patient outcomes, particularly in managing pain crises.
- Empowerment through cards – Distribution of over 26.2 million genetic status cards, enabling informed health and marital decisions for those with sickle cell trait.
- Transformative stories – Cases like Meena from Chhattisgarh, who accessed free treatment after sickle cell disease diagnosis, showcase grassroots impact and improvements in community health.
TECHNOLOGICAL AND COST INNOVATIONS
- PoC diagnostics – Adoption of point-of-care devices approved by ICMR for field-level testing of sickle cell disease in tribal belts, including solubility tests for rapid screening.
- Expanded approvals – From just 3 approved kits initially to over 30, significantly boosting accessibility for sickle cell screening and early diagnosis.
- Cost efficiency – Reduction in per-test cost from ₹100 to ₹28, enabling large-scale affordability of sickle cell testing.
- Rapid results – Quick turnaround ensures immediate initiation of treatment and counseling for sickle cell disease.
- Replicable model – Innovations provide a template for tackling other hereditary and rare diseases in rural India, including the implementation of newborn screening programs.
HOLISTIC CARE APPROACH
- Comprehensive care package – Free healthcare services, essential medicines, diagnostic facilities, and follow-up care for sickle cell disease patients, addressing the multifaceted needs of those with chronic illness, including management of chronic pain episodes.
- Therapeutic assurance – Hydroxyurea therapy provision reduces vaso-occlusive crises, need for blood transfusions, and improves quality of life for those with sickle cell anemia.
- Counseling priority – Premarital counseling integrated into health services to prevent future genetic transmission of sickle cell disease, especially important in communities where consanguineous marriages are common.
- Awareness generation – Use of community-level campaigns to promote understanding of sickle cell disease and early intervention, enhancing overall health awareness.
- Decision-making empowerment – Genetic status cards guide families in health planning and marriage choices, especially for those with sickle cell trait.
INSTITUTIONAL STRENGTHENING
- Centres of Excellence – 15 medical colleges and hospitals designated to handle complex sickle cell disease cases and provide prenatal diagnosis, enhancing the capabilities of healthcare providers.
- Specialist training – National Training of Trainers (ToT) programmes enhance capacity for sickle cell disease management and counseling, improving clinical management skills.
- Cross-ministry synergy – Collaboration between tribal affairs, social justice, education, women & child development for holistic outreach on sickle cell disease.
- Research-driven policy – Department of Health Research supports cost-effective, evidence-based interventions for sickle cell disease and other hemoglobin disorders.
- Infrastructure expansion – Specialised facilities established in high-burden districts for advanced diagnostics and treatment of sickle cell disease, strengthening overall healthcare infrastructure.
SOCIAL AND ETHICAL DIMENSIONS
- Equity focus – Addresses long-standing health disparities among tribal and marginalized ethnic groups affected by sickle cell disease.
- Cultural sensitivity – Health communication tailored to local languages and traditions builds trust in sickle cell disease interventions among indigenous populations.
- Women’s empowerment – Informed reproductive choices enhance maternal and child health outcomes in communities with high sickle cell prevalence.
- Community leadership – Local champions like Meena can serve as advocates and peer educators for sickle cell disease awareness, facilitating community outreach efforts.
- Ethical safeguards – Genetic data protection and informed consent remain essential for public trust in sickle cell screening programs, contributing to stigma reduction.
CHALLENGES AHEAD
- Awareness limitations – Lack of understanding and prevalence of myths hinder participation in sickle cell screening and counseling programmes.
- Geographic isolation – Tribal habitations often lack road connectivity, labs, and continuous medicine supply for sickle cell disease management, impacting primary healthcare delivery.
- Financial sustainability – Long-term funding is essential for free drugs, diagnostics, and awareness activities related to sickle cell disease.
- Workforce constraints – Shortage of trained doctors and genetic counselors in remote districts limits service reach for sickle cell disease care.
- Data management gaps – Inconsistent health record integration affects monitoring and evaluation of sickle cell disease programme outcomes and overall disease burden assessment.
WAY FORWARD
- Counseling expansion – Strengthen community-based premarital counseling to reduce intermarriage among sickle cell carriers and address issues related to consanguineous marriages.
- Awareness intensification – Engage local leaders, schools, NGOs, and social media to tackle stigma and misconceptions about sickle cell disease, enhancing overall health awareness.
- Research innovation – Invest in new drugs, gene therapy trials, and cost-effective testing kits for sickle cell disease and related hemoglobin disorders.
- Primary care integration – Embed sickle cell disease services into Ayushman Bharat Health and Wellness Centres, improving access to comprehensive care.
- Robust monitoring – Establish real-time data dashboards to guide adaptive policymaking for sickle cell disease control and track patient outcomes.
CONCLUSION
The NSCAEM demonstrates the transformative potential of political commitment, scientific innovation, and community participation in tackling hereditary blood disorders like sickle cell disease. Its comprehensive approach—covering screening, treatment, genetic counseling, and awareness—offers a model for other public health interventions. With sustained investment, robust community outreach, and adaptive policymaking, India is well-placed to eradicate sickle cell transmission by 2047, uplifting the health and dignity of millions, particularly among tribal populations. The mission’s success will be a testament to the nation’s resolve in achieving health equity for its most vulnerable citizens affected by sickle cell disease and other hemoglobin disorders.
SOURCE: HT
Mains Practice Question:
“The National Sickle Cell Anaemia Elimination Mission aims to address a major public health challenge in India’s tribal regions. Evaluate its achievements, innovations, challenges, and the steps needed to meet its 2047 elimination target.”