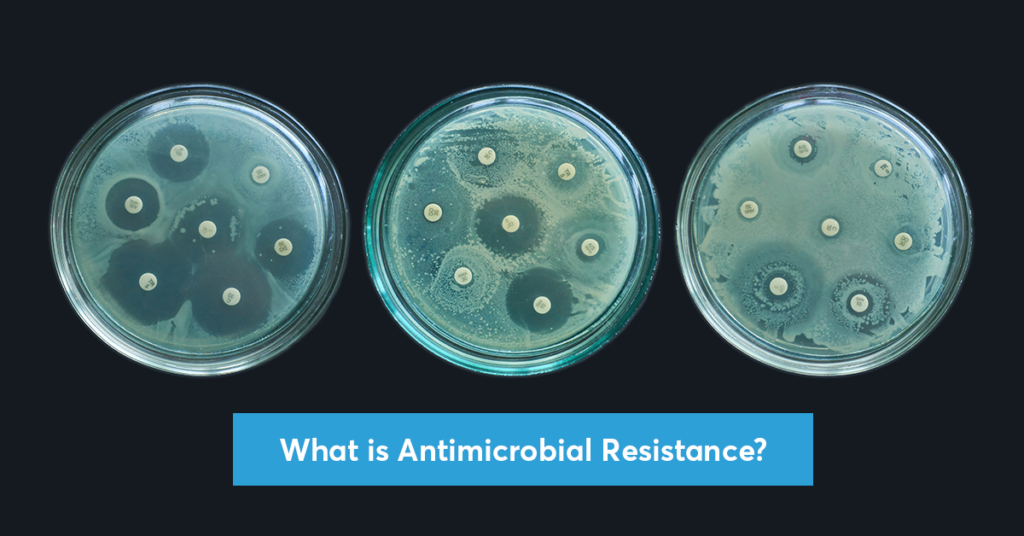
Vaccines Key To Combating India’s Antibiotic Resistance
Vaccines Key To Combating India’s Antibiotic Resistance
Syllabus:
GS-2: Government Policies & Interventions
GS-3: Health
Why in the News ?
India is witnessing a severe Antimicrobial Resistance (AMR) crisis, with drug-resistant infections causing thousands of deaths annually. A recent report by the Global Antibiotic Resistance Partnership (GARP) highlighted that expanding vaccination coverage, especially for typhoid and pneumonia, can significantly reduce antibiotic consumption and slow the rise of resistance.
India’s Growing Antibiotic Resistance Crisis:
Rising Burden
- India records the highest number of AMR-related deaths globally.
- Around 67 lakh deaths in 2021 were directly caused by drug-resistant infections.
- Nearly one million additional deaths were associated with antibiotic resistance.
Hospital-Level Threat
- Drug-resistant infections are increasingly common in hospital wards.
- Resistance to advanced antibiotics such as carbapenems has emerged in India.
- Such antibiotics are often expensive and inaccessible for poor households.
Typhoid Concern
- Surveillance data between 2017–2020 showed high typhoid incidence:
- Vellore – 1,173 cases per 100,000 child-years
- Kolkata – 714 cases
- Delhi – 576 cases
- Salmonella typhi strains resistant to major antibiotics are spreading rapidly.
Public Health Implications
- Resistant infections increase:
- Treatment costs
- Hospital stay duration
- Mortality rates
- AMR threatens decades of progress in modern medicine.
Global Dimension
- WHO has classified AMR among the top global health threats.
- Developing nations like India face the greatest burden due to:
- Poor sanitation
- Unregulated antibiotic sales
- Weak healthcare systems
Understanding Antimicrobial Resistance And Vaccination Provisions:Important points● India has the world’s largest AMR burden. ● WHO estimates vaccines can reduce 22% of global antibiotic use. ● Mission Indradhanush launched in 2014. ● India introduced PCV in 2017. Important Vaccines● Typhoid Conjugate Vaccine (TCV) ● Pneumococcal Conjugate Vaccine (PCV) Important Organisations● WHO ● Global Antibiotic Resistance Partnership (GARP) ● One Health Trust ● National Technical Advisory Group on Immunization (NTAGI) Important Concepts● Antimicrobial Resistance (AMR) ● Antibiotic Stewardship ● One Health Approach ● Universal Immunisation Programme (UIP) Government Initiatives● Mission Indradhanush ● National Action Plan on AMR (2017-2021) ● Ayushman Bharat Relevant International provisions● WHO Global Action Plan on AMR ● Sustainable Development Goal (SDG)-3: Good Health and Well-being |
Link Between Antibiotic Misuse And Resistance
Overuse Problem
- Antibiotics are frequently prescribed for:
- Viral fevers
- Common coughs
- Diarrhoea
- Such unnecessary use accelerates bacterial resistance.
Easy Availability
- Over-the-counter sale of antibiotics remains widespread.
- Weak pharmacy regulation encourages self-medication.
Underuse Equally Dangerous
- In rural India, many patients cannot:
- Afford antibiotics
- Complete treatment courses
- Incomplete treatment promotes resistant bacterial strains.
Urban-Rural Divide
- Urban India suffers from antibiotic overconsumption.
- Rural India faces limited access to proper healthcare.
Selection Pressure
- Frequent antibiotic use creates selection pressure.
- Resistant bacteria survive and multiply while normal strains die.
Vaccination As A Powerful AMR Solution
Preventing Infection
- Vaccines stop diseases before infection occurs.
- Reduced infections mean:
- Fewer antibiotic prescriptions
- Lower resistance development
WHO Estimates
- WHO states that optimal vaccine use could reduce:
- 5 billion daily antibiotic doses annually
- Nearly 22% of global antibiotic consumption
Typhoid Conjugate Vaccine (TCV)
- India already has four licensed TCVs.
- Three are WHO-prequalified and manufactured domestically.
High Effectiveness
- TCV provides nearly 85% protection against confirmed typhoid cases in children.
Low-Cost Intervention
- Delivery cost in Navi Mumbai is estimated below 55 US cents per dose.
- Makes vaccination economically viable at large scale.
India’s Missed Opportunities In Vaccine Deployment
Delay In National Rollout
- The National Technical Advisory Group on Immunization recommended TCV rollout in 2022.
- India has still not integrated it into the national immunization programme.
Global Comparisons
- Countries already adopting TCV include:
- Pakistan
- Nepal
- Zimbabwe
- Burkina Faso
Pneumonia Vaccination Gap
- Pneumococcal Conjugate Vaccine (PCV) introduced in India only in 2017.
- Rollout came much later compared to global standards.
Adult Vaccination Neglected
- No routine public-sector vaccination for:
- Adults above 65 years
- High-risk populations
Evidence Of Success
- One Health Trust study showed:
- Reduced antibiotic consumption
- Lower infection burden after PCV introduction
India’s Immunisation Achievements And Limitations
Mission Indradhanush Success
- Launched in 2014 to improve immunization coverage.
- Full immunization rose:
- From 62% (2015-16)
- To 76% (2019-21)
Strong Infrastructure
- India possesses:
- Large vaccine manufacturing base
- Established cold-chain network
- Massive healthcare workforce
Regional Disparities
- Vaccination coverage remains below 60% in several northeastern states.
Child-Centric Approach
- Immunisation programmes focus largely on children.
- Adult vaccination remains poorly developed.
Need For Strategic Shift
- Vaccination should be viewed as:
- A national AMR strategy
- Not merely a child welfare programme
Challenges In Tackling AMR Through Vaccination
Policy-Level Challenges
- Delay in incorporating TCV into Universal Immunisation Programme.
- Lack of a dedicated national strategy linking vaccination with AMR control.
- Weak coordination between health ministries and state governments.
Healthcare Infrastructure Issues
- Poor healthcare access in rural and tribal areas.
- Inadequate cold-chain facilities in remote regions.
- Shortage of trained healthcare workers for adult immunisation.
Financial Constraints
- Public health expenditure remains below desired levels.
- Adult vaccination programmes require substantial funding support.
- High out-of-pocket healthcare expenses discourage preventive care.
Awareness Deficit
- Limited public awareness regarding:
- Vaccine benefits
- Dangers of antibiotic misuse
- Vaccine hesitancy persists in some communities.
Regulatory Weakness
- Continued over-the-counter sale of antibiotics.
- Weak monitoring of prescription practices.
- Lack of strong antibiotic stewardship programmes.
Data And Surveillance Problems
- Limited real-time AMR surveillance systems.
- Underreporting of resistant infections in rural areas.
- Insufficient research on vaccine impact on antibiotic consumption.
Way Forward For India’s Vaccine-Based AMR Strategy
Expand Vaccine Coverage
- Immediately include Typhoid Conjugate Vaccine in UIP.
- Extend Pneumococcal vaccination to:
- Elderly population
- High-risk adults
Strengthen Adult Immunisation
- Develop a national adult vaccination policy.
- Integrate vaccination into primary healthcare systems.
Improve Awareness
- Launch nationwide campaigns on:
- Rational antibiotic use
- Importance of preventive vaccination
Enhance Surveillance
- Build stronger AMR monitoring systems.
- Expand genomic surveillance of resistant pathogens.
Regulate Antibiotic Sales
- Strict enforcement against non-prescription antibiotic sales.
- Promote antibiotic stewardship in hospitals.
Boost Public Health Investment
- Increase healthcare spending on:
- Vaccines
- Research
- Rural healthcare delivery
Adopt One Health Approach
- Integrate human, animal, and environmental health strategies.
- Reduce antibiotic misuse in livestock and agriculture.
Conclusion:
India’s fight against Antimicrobial Resistance cannot rely solely on restricting antibiotics. Preventing infections through widespread vaccination offers a sustainable and cost-effective solution. With strong vaccine manufacturing capabilities and existing immunisation infrastructure, India possesses the tools needed to curb AMR. Political commitment and expansion of adult immunisation are now essential.
Source: HT
Mains Practice Question:
“Vaccination can become India’s most effective weapon against rising antimicrobial resistance.” Examine the role of vaccines in reducing antibiotic dependence and discuss the challenges in integrating vaccination into India’s broader AMR strategy. (250 words)