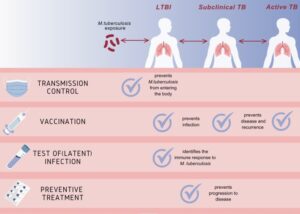
India’s 5 Pathways to Eliminate Tuberculosis
India’s Five Priority Pathways to Eliminate Tuberculosis
Syllabus:
GS Paper-2 Health ,Government Policies & Interventions, Important International Institutions
Why in the News ?
India has made significant progress in reducing tuberculosis (TB) cases, achieving a 21% decline in the last decade. However, with over 3 lakh annual deaths and rising urban and tribal burdens, renewed focus on targeted interventions, diagnostics, and research is essential to meet India’s goal of TB elimination by 2025.
Progress in India’s TB Elimination Efforts :
- Case Reduction: India reduced TB incidence by 21%, outperforming global averages.
- Increased Detection: Over 26 lakh cases in 2025 indicate improved identification of “missing patients.”
- Policy Commitment: Sustained political will and funding under National TB Elimination Programme (NTEP).
- Technological Adoption: Use of AI-based X-rays, molecular diagnostics, and community screening.
- Global Leadership: India emerging as a leader in TB innovation for Global South countries.
About Tuberculosis :
Important points
- Caused by Mycobacterium tuberculosis
- Spread through airborne droplets
- India has the highest TB burden globally
- TB is curable and preventable
- High-risk groups: HIV patients, diabetics, malnourished, migrants
Government Programmes
- National TB Elimination Programme (NTEP)
- Nikshay Portal: Digital TB tracking system
- Nikshay Poshan Yojana: Nutritional support to TB patients
- TB Harega Desh Jeetega Campaign
Global Initiatives
- WHO End TB Strategy (2015–2035)
- Sustainable Development Goal (SDG 3.3): End TB epidemic
Important Acts/Institutions
- Indian Council of Medical Research (ICMR)
- Anusandhan National Research Foundation (ANRF)
- District Mineral Foundation (DMF) under MMDR Act
Reducing TB Mortality through Targeted Care :
- High Mortality Concern: Over 3 lakh deaths annually despite TB being curable.
- Early Death Risk: Majority deaths occur within 2 months of diagnosis, especially first two weeks.
- Differentiated TB Care: Focus on high-risk patients with comorbidities like HIV, diabetes, malnutrition.
- TN-KET Model: Tamil Nadu initiative reduced deaths by 10% overall, 20% early fatalities.
- Holistic Support: Need for nutrition, de-addiction services, and district-level hospital beds.
Closing Diagnostic Gaps :
- Subclinical TB Challenge: Nearly 50% cases asymptomatic, contributing to silent transmission.
- Community Screening: Expansion of doorstep screening strategies.
- Technological Innovation:
○ Portable AI-powered X-rays
○ Tongue/nasal swab tests
○ Open PCR systems (80% cheaper)
- COVID Infrastructure Use: Repurposing lab networks built during pandemic.
- Affordability Focus: Indigenous technologies reducing diagnostic costs significantly.
Addressing Vulnerable Populations :
- Tribal Burden: TB prevalence among Scheduled Tribes is 50% higher than others.
- Socio-economic Determinants: Poverty, malnutrition, and poor access to healthcare.
- Targeted Policies: Need for region-specific interventions.
- Institutional Mechanisms: Dedicated subcommittees for tribal and marginalized areas.
- Funding Opportunities: Use of District Mineral Foundation (DMF) funds in mining regions.
Tackling Urban TB Hotspots :
- Urban Risk Factors: High population density, migration, slum conditions, and lack of pollution free environment contribute to respiratory vulnerabilities.
- Governance Gap: National programmes insufficient without Urban Local Bodies (ULBs) involvement.
- Decentralised Action: Integrating TB into municipal health planning, particularly in coastal regulation zone areas with dense populations.
- Swachh Bharat Model: Demonstrates effectiveness of local governance mobilisation.
- Resource Availability: Increased central grants to ULBs can support TB initiatives.
Strengthening Research and Innovation :
- Research Ecosystem Boost: Establishment of Anusandhan National Research Foundation (ANRF).
- ICMR Leadership: Potential to lead a TB Accelerator platform.
- Focus Areas:
○ New vaccines
○ Advanced diagnostics
○ Effective drug regimens
○ Environmental impact assessment of healthcare infrastructure
- Collaborative Approach: Public-private-philanthropic partnerships.
- Global Impact: Development of affordable solutions for high-burden countries.
Financing and Governance Innovations :
- Untapped Funds: ₹21 lakh crore corpus under DMF, 60% unspent.
- Reallocation Potential: Even small allocation can boost TB diagnostics and screening. DMF funds, primarily collected from mining activities requiring environmental clearances under the Forest Conservation Act, can be strategically redirected toward health infrastructure in tribal and mining-affected regions.
- Best Practice Example: Chamarajanagar (Karnataka) investing in diagnostics while ensuring compliance with environmental clearance norms for new healthcare facilities.
- Accountability Mechanisms: Localised monitoring through Panchayati Raj and ULBs, incorporating principles of environmental democracy and the precautionary principle in public health governance.
- Time-bound Roadmap: Need for measurable targets and accountability frameworks, avoiding ex post facto approvals that delay implementation.
Challenges :
- High Mortality Rate: Despite treatment availability, late diagnosis and weak follow-up lead to preventable deaths.
- Diagnostic Gaps: Large proportion of asymptomatic cases remain undetected, sustaining transmission.
- Healthcare Inequity: Tribal and urban poor face limited access to healthcare services.
- Urban Complexity: Migration, informal settlements, and overcrowding complicate disease tracking and treatment adherence.
- Social Determinants: Malnutrition, alcohol use, and co-morbidities worsen TB outcomes.
- Funding Utilisation Issues: Available funds like DMF remain underutilised, sometimes due to delays in obtaining retrospective environmental clearances for infrastructure projects.
- Fragmented Governance: Lack of coordination between central, state, and local bodies, with post facto policy adjustments creating implementation gaps.
- Research Gaps: Limited investment in next-generation vaccines and drugs.
- Stigma and Awareness: TB patients face social stigma, delaying treatment seeking.
- Operational Challenges: Weak last-mile delivery in remote and underserved areas.
- Environmental Factors: Industrial pollution and poor environmental conditions in mining regions exacerbate respiratory health issues, necessitating application of the polluter pays principle.
Way Forward :
- Patient-Centric Care: Scale up Differentiated TB Care for high-risk individuals.
- Universal Screening: Expand community-based and AI-supported screening nationwide.
- Strengthen Diagnostics: Promote indigenous technologies and decentralised testing.
- Targeted Interventions: Develop region-specific strategies for tribal and urban populations, incorporating environmental jurisprudence principles in health policy formulation.
- Local Governance Role: Empower ULBs and Panchayats with funds and accountability mechanisms, drawing lessons from environmental democracy frameworks and the Vanashakti judgment on participatory governance.
- Optimal Fund Utilisation: Redirect DMF and other untapped funds towards TB programmes, ensuring streamlined processes that avoid ex-post facto clearances and delays.
- Nutritional Support: Integrate nutrition, mental health, and addiction services into TB care.
- Research Investment: Strengthen ANRF and ICMR-led initiatives for innovation, including studies on environmental determinants of TB.
- Public Awareness Campaigns: Reduce stigma and promote early diagnosis and adherence.
- Time-bound Targets: Establish district-level monitoring systems with clear milestones, incorporating EIA notification principles for new healthcare infrastructure to ensure sustainable development.
- Holistic Approach: Adopt the precautionary principle in public health planning, ensuring that TB elimination efforts are integrated with broader environmental and social determinants of health.
Conclusion :
India has achieved notable success in reducing TB but must now shift focus towards reducing deaths, bridging diagnostic gaps, and targeting vulnerable populations. With strong political will, technological innovation, and decentralised governance that incorporates principles of environmental democracy and sustainable development, India can transform its TB elimination goal into reality and set a global benchmark. The integration of health and environmental governance frameworks, including proper utilization of DMF funds with appropriate environmental clearances, will be crucial in achieving a pollution free environment conducive to respiratory health and overall TB elimination.
Source:HT
Mains Practice Question :
“Despite significant progress, tuberculosis remains a major public health challenge in India.” Discuss the key priorities required to eliminate TB in India. Also examine the role of technology, local governance, and targeted interventions in achieving the goal of TB elimination by 2025.